Glaucoma is a group of sight threatening eye diseases which reduces your peripheral vision.
It is one of the most common eye diseases in the UK and in the early stages you have no symptoms.
The condition occurs when the optic nerve in the back of the eye gets damaged, typically as a result of raised pressure within the eye. Modern treatment options attempt to prevent glaucoma from progressing, but cannot repair damage which has already occurred and therefore it is beneficial to diagnose and treat the disease in the early stages.
Earlam and Christopher director Edward Farrant has particular interests in acute eye care and glaucoma and he works regularly at both Musgrove Park Hospital and Bristol Eye Hospital as a glaucoma shared care optometrist. He has completed a number of specialist exams in glaucoma and therapeutics, and is one of only a handful of expert practitioners across the whole country
Acute angle-closure Glaucoma Acute angle-closure glaucoma develops rapidly. Symptoms are often severe. They include:
- Intense pain
- Redness of the eye
- Headache
- Tender eye area
- Seeing halos or ‘rainbow-like’ rings
- Around lights
- Misty vision
- Loss of vision in one or both eyes that
- Progresses very quickly
Glaucoma is caused by a blockage in part of the eye. This prevents fluid draining out of the eye and increases pressure in the eye, called intraocular pressure.
There are a number of things that can increase your risk of developing glaucoma:
Age – glaucoma becomes more likely as you get older. In the UK, chronic open-angle glaucoma affects one to two people in every 100 who are over 40 years old, and four to five people in every 100 who are over 80 years old
Ethnic origin – people of African or Afro-Caribbean origin are at increased risk of developing chronic open-angle glaucoma. People of Asian origin are at increased risk of developing acute angle-closure glaucoma
Short sightedness (myopia) – people who are short-sighted are more likely to develop chronic open-angle glaucoma
Ocular hypertension (OHT – raised pressure in the eye) – People with OHT are at increased risk of developing chronic open-angle glaucoma. Your optometrist will be able to diagnose OHT (see diagnosing glaucoma)
Family history – if you have a close relative, such as a parent, brother or sister who has glaucoma, you are at increased risk of developing the condition yourself
Medical history – people with diabetes, which is a condition caused by too much glucose in the blood, may be at increased risk of developing glaucoma
The first thing we need is to consult with you and complete an eye examination, and with nationally renowned experts in our practice you’ll find this service thorough and professional.
Your Examination may or will include:
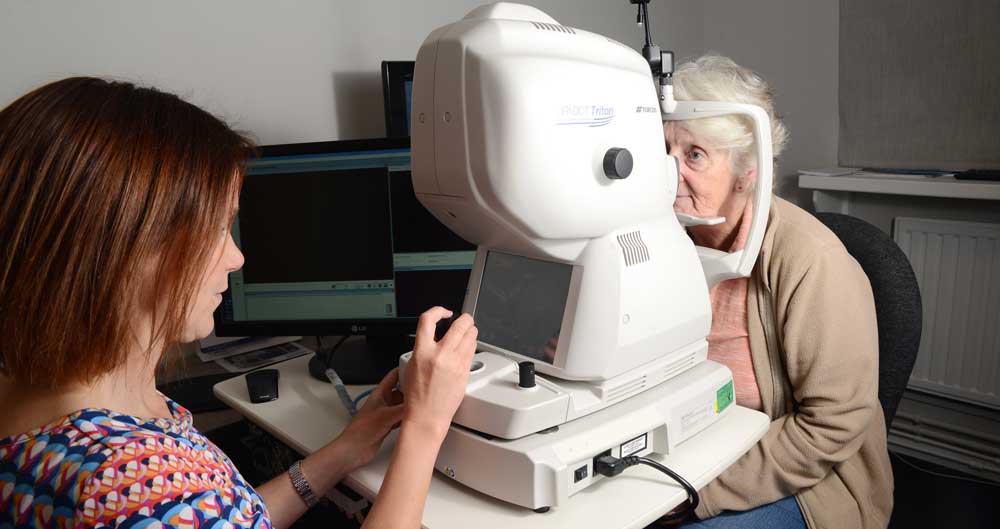
Our state of the art OCT takes 3D cross sectional scans of the optic nerve in the back of your eyes. This allows us to very accurately monitor your eye health, allowing us to pick up any subtle changes with your optic nerves
Gonioscopy
This specialist technique allows us to examine and monitor the drainage part of your eye, which can become blocked in glaucoma causing the pressure to rise.
Central Corneal Thickness (Pachymetry)
This is a technique using ultrasound that allows us to accurately measure the thickness of your cornea. This measurement allows us to be very accurate in determining your eye pressure and also look for signs that can put people more at risk of the disease.
Detailed Visual Field Analysis
Our Visual field testing uses the latest hospital equipment to accurately detect and monitor changes with your vision.
If there appears to be an issue that can be managed through medication then are dispensing team will be able to prescribe the right product for you. If the situation is more serious we can advise on the next steps, such as recommending you to a hospital but this is rare.
Ocular Hypertension is a condition in which a higher than average pressure is present in your eyes, without the nerve damage typical in glaucoma.
People with ocular hypertension are more at risk of developing glaucoma and therefore require regular monitoring. In some cases they may require treatment, usually in the form of eye drops to reduce the risk of developing glaucoma in the future.
As there are no symptoms with ocular hypertension it is impossible for a individual person to notice it on their own. But with a regular eye examination schedule an eye care professional can find it in routine testing.
During a regular eye exam, intraocular pressure is measured using a device called a tonometer. If elevated pressure is measured above a certain level you may be diagnosed with ocular hypertension.
As ocular hypertension is closely linked to glaucoma there are a number of things that can increase your risk of developing ocular hypertension:
Age – ocular hypertension and glaucoma becomes more likely as you get older.
Ethnic origin – people of African or Afro-Caribbean origin are at increased risk of developing ocular hypertension and chronic open-angle glaucoma. People of Asian origin are at increased risk of developing acute angle-closure glaucoma and ocular hypertension
Short sightedness (myopia) – people who are short-sighted are more likely to develop ocular hypertension and chronic open-angle glaucoma
Family history – if you have a close relative, such as a parent, brother or sister who has glaucoma, you are at increased risk of developing the condition yourself
Medical history – people with diabetes, which is a condition caused by too much glucose in the blood, may be at increased risk of developing glaucoma
The first thing we need is to consult with you and complete an eye examination, and with nationally renowned experts in our practice you’ll find this service thorough and professional.
Your Examination may or will include:
Ocular Coherence Tomography
Our state of the art OCT takes 3D cross sectional scans of the optic nerve in the back of your eyes. This allows us to very accurately monitor your eye health, allowing us to pick up any subtle changes with your optic nerves
Gonioscopy
This specialist technique allows us to examine and monitor the drainage part of your eye, which can become blocked in glaucoma causing the pressure to rise.
Central Corneal Thickness (Pachymetry)
This is a technique using ultrasound that allows us to accurately measure the thickness of your cornea. This measurement allows us to be very accurate in determining your eye pressure and also look for signs that can put people more at risk of the disease.
Detailed Visual Field Analysis
Our Visual field testing uses the latest hospital equipment to accurately detect and monitor changes with your vision.
If there appears to be an issue that can be managed through medication then are dispensing team will be able to prescribe the right product for you. If the situation is more serious we can advise on the next steps, such as recommending you to a hospital but this is rare.
